 Successively, it runs along the free margin of the tentorium and then enters the cavernous sinus, inferior to the III nerve and superior to the ophthalmic division of the V nerve. After exiting the pons, the nerve curves over the superior cerebellar peduncle and then runs between the SCA and the PCA. It is the unique nerve with a root zone arising from the posterior brainstem where its nucleus lies. The trochlear nerve innervates only the superior oblique muscle. Successively, the nerve enters in the cavernous sinus where is the most superior nerve, to reach the orbit through the superior orbital fissure (Fig. The nerve emerges from the interpeduncular cistern running through the perimesencephalic cistern, superiorly to the posterior cerebral artery (PCA) and inferiorly to the superior cerebellar artery (SCA). The parasympathetic fibers arise in the Edinger-Westphal nucleus, situated dorsally to the oculomotor nuclear complex. Somatic motor fibers of oculomotor originate from the nuclear complex located in the midbrain at the level of the superior colliculi, ventral to the cerebral aqueduct and the periaqueductal gray matter. The oculomotor nerve has a somatic motor function of most ocular estrinsic muscles (inferior, superior, middle rectus, inferior oblique, and levator palpebrae superior muscles) and a parasympathetic function (ciliaris and sphincter pupillae muscles). įull size image III cranial nerve - Oculomotor nerve Particularly, CT is optimal to study the bony foramina of the skull base (Table 3, Fig. Therefore, it can be useful to evaluate the intraosseous segments of cranial nerves and the possible associated bony changes. CT is inferior to MRI in the visualization of the cranial nerves themselves, due to its low contrast resolution. MRI could also be useful to assess denervation changes of “end-organ muscles” (Table 2). 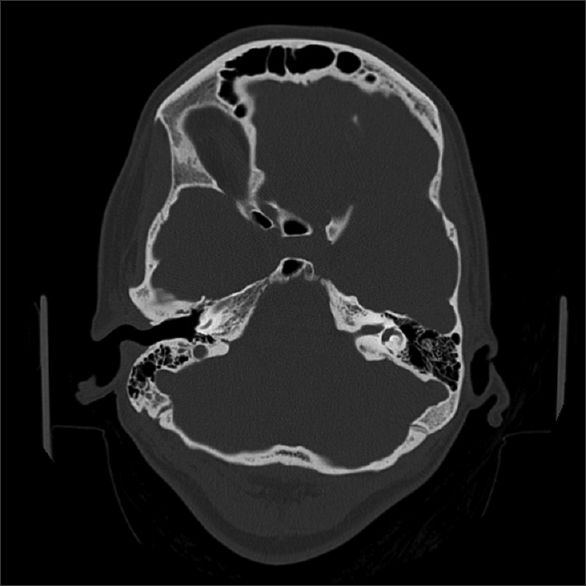
Three-dimensional T1-weighted gradient echo sequences can provide a better visualization of the nerve enhancement, surrounded by CSF. The enhancement of the nerve, after gadolinium administration, is associated to disruption of the blood-nerve barrier and may be secondary to neoplasm, inflammation, demyelination, ischemia, trauma, radiation treatment, and axonal degeneration. These sequences typically show dark cranial nerves against a background of bright CSF (Fig. Several scientific articles have underlined the importance of SSFP sequences for the visualization of the cisternal spaces of cranial nerves thanks to their sub-millimetric spatial and high contrast resolution. Table 1 summarizes the most important sequences and features in their study. 
MRI is considered the gold standard in the study of cranial nerves. We believe that it could be a useful guide for radiologists and neuroradiologists to review the anatomy and the most important pathologies that involve cranial nerves and their differential diagnosis. The article is a complete pictorial overview of the imaging of cranial nerves, with anatomic and pathologic descriptions and great attention to illustrative depiction. Computed tomography (CT) allows, usually, an indirect view of the nerve and is useful to demonstrate the intraosseous segments of cranial nerves, the foramina through which they exit skull base and their pathologic changes. Magnetic resonance imaging (MRI) is considered the gold standard in the study of the cranial nerves. Cranial nerve dysfunctions may be the result of pathological processes of the cranial nerve itself or be related to tumors, inflammation, infectious processes, or traumatic injuries of adjacent structures. Therefore, it is necessary to know the most frequent pathologies that may involve cranial nerves and recognize their typical characteristics of imaging. The anatomy of cranial nerves is complex and its knowledge is crucial to detect pathological alterations in case of nervous disorders. The human body has 12 pairs of cranial nerves that control motor and sensory functions of the head and neck. 
0 Comments
Leave a Reply. |



 RSS Feed
RSS Feed
